 By Jeremy Collins, MD
By Jeremy Collins, MD
Quality Outcomes Division Councilor
SIR Foundation
On May 9, 2016, the proposed Medicare Access and Children’s Health Insurance Program Reauthorization Act (MACRA) rule was published providing details regarding how the Center for Medicare and Medicaid Services (CMS) anticipates scoring providers through the Merit-based Incentive Payment System (MIPS). Starting in 2017, MIPS replaces several CMS programs including the Physician Quality Reporting System (PQRS), Physician Value-based Payment Modifier (VM) and the Medicare electronic health record (EHR) incentive program for eligible professions. MIPS scores will influence incentive payments two years ahead (i.e., MIPS performance in 2017 will influence incentive payments in 2019).
The MIPS program scores eligible clinicians across four separate categories: quality measures, resource use, clinical practice improvement activities (CPIA) and advancing care information. Scores on all four of these components are tallied, yielding a MIPS composite score. CPIAs, the focus of this article, is weighted at 15 percent of the composite score and represents a new measurement category for CMS. Al though CPIAs are aligned with the American Board of Radiology’s Maintenance of Certification Part IV: Practice Quality Improvement requirements, there are additional requirements to consider to score well on the CPIA part of MIPS.
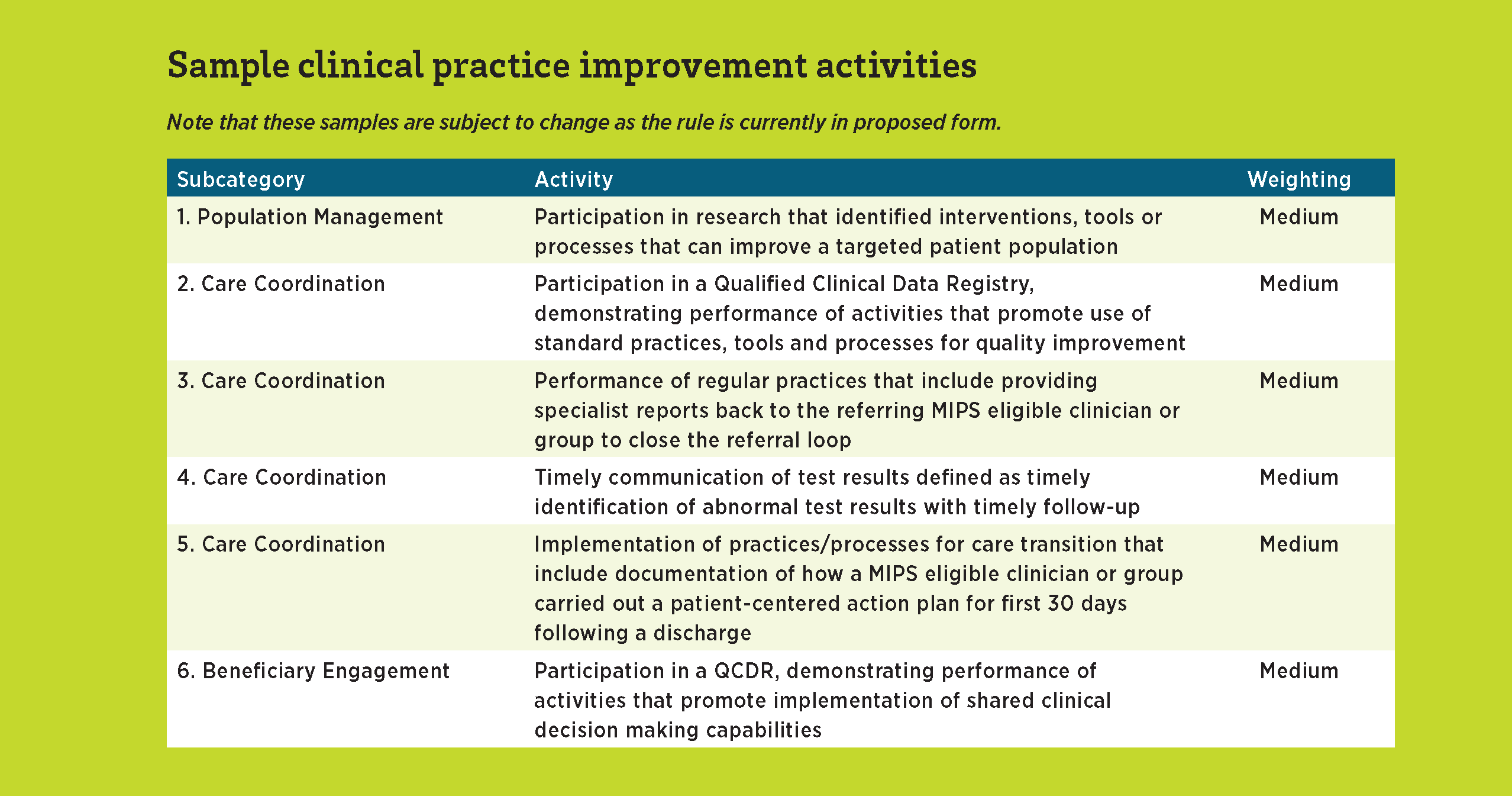
CMS defines a CPIA as “an activity that relevant eligible clinician organizations and other relevant stakeholders identify as improving clinical practice or care delivery and ... when effectively executed is likely to result in improved outcomes.” CMS has defined 94 such activities in the inventory of the proposed rule and has detailed an annual process whereby stakeholders can propose new CPIAs. This process opens in 2017 for potential inclusion in the 2018 MIPS program. Broad categories for CPIAs include expanded practice access, population management, care coordination, beneficiary engagement, patient safety and practice assessment, and participation in an alternative payment model (APM). In addition, the following three categories are being considered for inclusion in the final rule: emergency preparedness and response, integration of primary care and behavioral health, and achieving health equity. The CPIA inventory is provided in Appendix H of the proposed rule.
Based on a particular provider’s classification as a qualified advanced alternative payment model (APM) participant, partial qualifying APM participant or MIPS eligible clinician there are different reporting requirements and scoring schemata applied to CPIA. At present, SIR anticipates that most IRs will be classified as MIPS eligible clinicians.
The number of CPIAs required during each yearlong reporting period (Jan. 1–Dec. 31) depends on the MIPS eligible clinician classification as “patient-facing” vs. “non-patient facing.” Although the CMS definition of “patient-facing” is evolving, IRs would be classified as “patient-facing” if they see at least 25 specifically coded encounters. Patient-facing eligible clinicians in groups of > 15 clinicians or those who do not meet the CMS definition of rural practice group have a maximum total of 60 points with medium- and high-level activities credited at 10 and 20 points, respectively. Each CPIA has to be reported for at least 90 days in a reporting period to receive credit.
“Non-patient facing” clinicians, small group practices of greater than 15 clinicians or those in rural areas only need to report on two CPIAs per reporting period, with equal weighting of 30 points to each. It is important to note that while there are reduced reporting requirements for non-patient facing clinicians for CPIAs at the outset of the MIPS program, the proposed rule contains language noting that the feasibility of additional CPIA reporting will be reconsidered for such physicians going forward. Also at the outset of the program CPIA credit is awarded for participation, rather than for documenting a performance improvement over the baseline rate.
CMS has proposed a wide range of CPIA reporting mechanisms, including qualified registries, qualified clinical data registries (QCDRs), electronic health records (EHRs), attestation and administrative claims. Although the feasibility of such reporting mechanisms depends on the CPIA selected and the definitions of performance within each, this maximizes reporting options for eligible clinicians. SIR is exploring CPIA reporting options to streamline the reporting process for members.
The society is working to comment on the proposed rule, including the available CPIA inventory for the 2017 performance year. The final rule will be published in fall 2016. Resources are available for SIR members to learn more about MACRA:
• Volunteers are updating the IR Quality Toolkit (free for SIR members) to reflect the new era of health care economics that has been ushered in by the repeal of the sustainable growth rate and MACRA. The IR quality toolkit will be updated later this year to reflect the content of the MACRA final rule providing a summary of the legislation for membership.
• Interested members are encouraged to plan to attend a dedicated day-long session on health care reform, quality, reporting and practice management held at the upcoming SIR 2017 Annual Meeting in Washington, D.C.
• SIR has compiled an online collection of MACRA resources.
• Further MACRA updates and analyses will appear in upcoming issues of IRQ.
This article was adapted from the summer edition of IR Quarterly. Log in to read the full issue online here.